This is just a quick post to alert those who do not yet know about the DFID consultation on reproductive, maternal and newborn health, and to remind those who have not yet commented, that the deadline for participation in this important consultation is 20October.
This consultation is particularly important given the recent high level discussions on progress towards the Millennium Development Goals (MDGs) at the UN Summit last month, which highlighted slow progress in reducing maternal mortality.
The background to this consultation is that MDG 5, which focuses on improving maternal health, is the most off-track MDG. Yet MDG 5 has a critical impact on the achievement of all the other MDGs. More than a third of a million women die every year from complications during pregnancy and childbirth. For every woman that dies another 20 women suffer from chronic ill-health or disability. In addition MDG 4, to reduce child mortality, is also off-track. More than eight million children die every year before their fifth birthday – at least 3.5 million of these deaths are of babies who die within the first month of life.
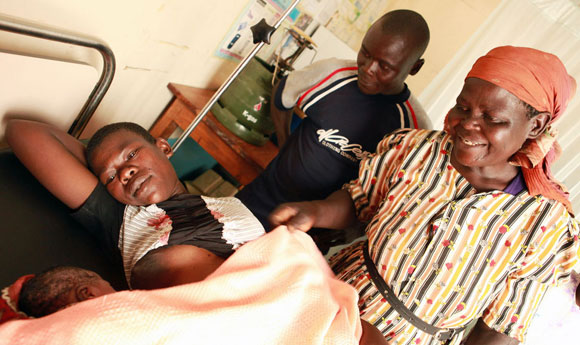
Improving reproductive, maternal and newborn health in the developing world is a major priority for the UK Government. DFID is therefore developing a new business plan, which will determine the UK’s contribution towards achieving MDG 5. We want to ensure that every pregnancy is wanted and that every birth is safe. In doing so, we know that we will also make an enormous contribution to reducing child mortality – particularly through improving the survival chances of newborn babies.
From the perspective of Mozambique, this is a high priority. The Government of Mozambique has recently estimated that the maternal mortality rate in Mozambique is over 500 per 100,000 live births. Whilst this is high, it is a significant improvement on the estimated rate in 2000. I have attached a link to a Population Reference Bureau article which highlights what the situation was like in 2000 and some of the challenges in both measuring and tackling maternal mortality.
In terms of the progress that has been made since then, there has been a significant increase in access to skilled attendance at delivery. Over 55% of mothers, or nearly 600,000 women, now give birth in a health institution with access to skilled care. The Government of Mozambique would like to increase the level of institutional deliveries to 66% by 2015, this will mean an extra 91,000 mothers per year having access to skilled care at delivery.
Another area where Mozambique intends to make progress is in access to modern methods of contraception. The 2008 Multiple Indicator Cluster Survey for 2008, which I have mentioned previously, indicated that in 2008 only 13.5% of Mozambican couples were using a modern method of contraception. Evidence produced in the Lancet suggests that promotion of family planning could reduce maternal deaths by 32% and childhood deaths by 10%. Due to the increased space between births and therefore the health of mothers and children, and the avoidance of unwanted pregnancies and the risk of unsafe abortion, which remains a major cause of mortality in many developing countries. Current government plans are to increase the contraceptive prevalence level to 19% by 2015, this would increase the number of women using contraception by 276,000 per year.
However the national plan for achieving MDGs 4 and 5 includes a more ambitious target of a contraceptive prevalence of 30%, which is considered necessary in order to reduce maternal mortality below 400 per 100,000. Whether this will be achieved will depend on overall levels of funding, and whilst funding at the international level for maternal and child health has increased in recent years, significant investment at the country level remains a priority.
But enough from me, your comments on the DFID consultation would be most welcome.

Recent Comments