I am writing this sitting in Johannesburg airport on my way back from a fascinating week in South Africa, where I have been conducting a review of a UK aid supported programme on maternal and child health. The programme supports the Government of South Africa’s strong commitment to bring down its high maternal, newborn and child mortality rates.
It has been a packed, tiring, but fascinating week which has opened my eyes to some of the huge challenges and persisting inequalities that face the people of South Africa and their healthcare system. South Africa, like Malawi which I recently visited, is a country where HIV is having a massive impact on health.

After arriving in Pretoria, red eyed and sleepless on a Monday after a night sitting on a plane, I had just 30 minutes for a shower before the first meeting of the day. However, energy levels were soon recharged by the enthusiasm and commitment of the people I met working on these issues.
One of the first people I spoke to was Dr. Nat Khaole (pictured), the Director of Maternal Child and Women’s Health in the National Department of Health. With an encyclopedic knowledge of his subject area, Dr. Khaole highlighted many of the challenges facing South Africa as it tries to deliver the commitments the Minister of Health made to the President in the Negotiated Service Delivery Agreement. The commitments are: to increase life expectancy, reduce maternal and child mortality, combat HIV/AIDS and TB and to strengthen the health system.
In this post, I will briefly profile the ‘Essential Steps in Managing Obstetric Emergencies’ (ESMOE) project, which is run jointly by the University of Pretoria with support from the Liverpool School of Tropical Medicine and Hygiene under the supervision of the National Department of Health.
The Maternal Mortality Ratio (MMR) in South Africa is incredibly high 310/100,000 – a figure similar to other countries in Sub-Saharan Africa, but surprising for South Africa given its level of development and gross domestic product level, which at about $11,000 is much higher than most other Sub-Saharan countries.
Part of the explanation for South Africa’s high maternal mortality is the historic legacy of the apartheid years, where the level of service provision for the black majority of the population was much worse than that available to the white population, and with considerable urban rural differences. An excellent series of articles in the Lancet in 2009 give a real insight to the situation.
Investment to address this historic inequality is ongoing, but providing health services, trained staff, equipment and enabling access, particularly in remote and rural areas takes time. Like much of Africa, even with its higher level or resources, South Africa has struggled to train, deploy and retain enough doctors and nurses (a problem which is being highlighted by the Global Health Workforce Alliance). Making sure that the overworked staff who are present in facilities work in teams that have the skills needed to manage a complicated delivery of women struggling in labour, and to ensure the welfare of newborn children, is a challenge. The statistics posted below show life expectancy, maternal and neonatal mortality by year, with the target set for 2014, that the Government of South Africa hopes to achieve.
Table: Life expectancy and morality trends and targets 2009 – 2014.
| Indicator | Target 2014 | 2009 | 2010 | 2011 |
| Male life expectancy at birth (years) | 56 | 54 | 55.5 | 57.2 |
| Female life expectancy at birth (years) | 61 | 59 | 60.8 | 62.8 |
| Under 5 year Mortality Rate per 1000 live births | 50 | 56 | 53 | 42 |
| Infant Mortality Rate per 1000 live births | 36 | 40 | 37 | 30 |
| Neonatal Mortality Rate per 1000 live births | 12 | 14 | 13 | 14 |
| Maternal Mortality Ratio per 100,000 live births | 270 | 310 | 333 | ….. |
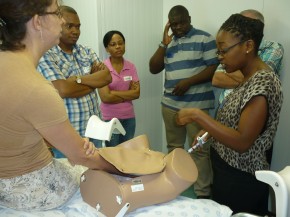
Professor Robert Pattinson, who is the Director of the Medical Research Council (MRC) Maternal and Infant Health Care Strategies Research Unit, at the University of Pretoria, and is the extremely knowledgeable and dedicated champion of the Essential Steps (ESMOE) project. I have posted a couple of pictures taken at a training session I attended whilst in South Africa, during a visit made to assess the quality of the programme. Here, doctors and nurses being trained use a mannequin to practice managing difficult births.
The project has identified the 15 districts in South Africa with the highest levels of maternal and newborn mortality. It has developed a 4 year programme with aims to train 80% of all health staff engaged in maternal health services with saturation training on obstetric and newborn care. The training materials build on knowledge gained in medical and nursing school, but use a hands on teaching method with mannequins and simulation of obstetric emergencies in order to fine tune the skills of health workers. (View a photo gallery about a similar programme in Sierra Leone).
The programme will be evaluating how effective the saturation training is compared to just having regular, in hospital simulation exercises for staff delivered by ‘Master Trainers’, also using mannequins.
It will take time to train all of the health workers, and for the full benefits of the programme to be realised. However, the 5th Confidential Enquiry into to Maternal Deaths report for the period 2008-2010 recognised the benefits of the training and made several recommendations about the importance of scaling up this training.
The potential prize is high. We hope to see reductions in maternal and infant mortality over the coming years as a result of expanded access of South Africans to treatment for HIV/AIDS, but hemorrhage and high blood pressure and preventable causes of death in pregnancy are killing South African mothers. This project will help HIV positive and HIV negative women alike.
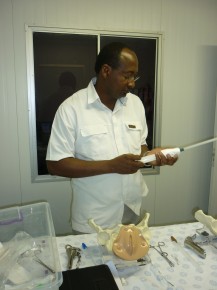
It was a real pleasure to meet Dr Mbisha (pictured) and other trainers at the training session in Sasolburg General Hospital. They are doing a great job that will make a real difference to the lives of South African mothers and children.

3 comments
Comment by Harriet Macdonald-Walker posted on
Really interesting Neil, thanks for sharing and for the links to the Lancet articles.
Best,
Harriet
Comment by domestic cleaning London posted on
Thanks for sharing Neil.
Comment by Zara A. posted on
This is really great job you've been done for the health problems in South Africa! As a person, coming from Australia I know how hard it could be to deal with such disease...
I've work in the cleaning industry for two years. With my team, we often meet many health problems because of people's ignorance and lack of knowledge of how to take care of themselves and their families. So, I would like to say that essential part of preventing many health issues is the clean and sanitised environment. As an expert, I've been working for many public facilities such as hospitals and laboratories. The sanitised process requires strict procedure - it is the firs step when fighting against all communicable diseases.